Written by Dr Shalen Sehgal | Crises Control CEO
Hospital incident response coordination is the part of emergency management that most facilities have not solved. The alert system? That works. In most hospitals today, a Code Blue notification reaches every registered device on the floor in under three seconds. The mass notification fires, the overhead page crackles, and every phone on the ward lights up.
And then nothing coordinates. Three people run to the same room with the same equipment. The respiratory therapist, who should be a critical part of the response, was never on the distribution list for this shift. The charge nurse who should be coordinating the response is still on hold waiting for a callback to confirm the attending physician got the message.
The alert worked. The coordination never started.
This is not a fringe scenario. It is what post-incident reviews find in hospital after hospital, regardless of investment in technology or quality of staff training. For what this looks like during a specific Code Blue, minute by minute, see the first five minutes of a hospital emergency. This post focuses on the coordination layer: what breaks it, why it keeps breaking, and what actually fixes it.
Why Hospital Incident Response Coordination Breaks After the Alert
Most investment in hospital emergency response has gone into the alert layer. Faster notifications. More channels. Better device coverage. The result is that alerts now arrive reliably and quickly.
But alert speed is not the bottleneck. It never was. The bottleneck is what happens in the 60 to 90 seconds after the alert lands and before the first coordinated action begins. That window has received almost no investment, because most tools were not designed to address it.
- Broadcasting to a group is not the same as assigning a task
When a Code Blue alert goes to the rapid response team as a group message, each member of that group has a rational expectation that someone else is handling it. This is not carelessness. It is the predictable consequence of a broadcast model. The message reached everyone. The task belongs to no one.
Effective hospital incident response coordination requires the opposite of broadcasting. It requires assigning a specific action to a specific person, tracking whether that person acknowledged it, and escalating automatically if they did not. Most hospital notification systems do none of these things.
- Delivery confirmation is not the same as response confirmation
A notification system that shows a delivered tick has told you the message reached a device. It has not told you whether the person saw it, whether they are available, whether they are moving, or whether they understood what they needed to do. In a clinical emergency, those are not details. They are the difference between a response that starts and one that stalls.
- Outdated contact lists create invisible gaps
Hospital rosters change constantly. Shift rotations, role changes, secondments, leave. The contact list that was accurate three months ago is not the same list that represents who is actually on the floor today. Hospital incident response coordination that routes alerts to named individuals rather than to current shift roles will reach the wrong people every time a staff member has moved on.
Research from TigerConnect found that improving code blue coordination across multiple hospital systems reduced team assembly time by an average of 78 seconds. At the University of Maryland Medical System, that improvement translated to patient survival rates rising from 17 percent to 25 percent. The same team. The same clinical capability. A better coordination system.
The Four Coordination Failures That Post-Incident Reviews Keep Finding
Healthcare incident investigators consistently identify the same four breakdowns, regardless of the type of incident, the size of the facility, or the level of investment in emergency technology.
1.No individual owns the first action
In a group notification, the task belongs to everyone collectively and therefore to nobody individually. Hospital incident response coordination only functions when each action is assigned to a specific person, with a specific deadline, and with automatic escalation if that person does not respond. Any system that stops at notifying the group has not started coordinating the response.
2.No one has a live view of the whole response
The charge nurse coordinating the response knows what she knows from her position. The administrator making decisions knows what the last phone call told her, which was 90 seconds ago. The attending physician, running from a different floor, does not know what has already been done by the time he arrives. Everyone is operating on partial, outdated information.
3. Escalation is manual and slow
When a critical responder does not acknowledge their notification, someone has to notice, decide to follow up, find the backup contact, and reach them. In the meantime, the incident is progressing. Manual escalation is a human-speed process in a situation that is moving faster than humans can reliably track.
4.The documentation happens after the fact
CMS, the Joint Commission, and HIPAA all require contemporaneous evidence of the response: who was notified, when, how they responded, what actions were taken. In most facilities, this record is compiled from memory after the incident closes. It is never entirely accurate. The incident management platform that logs every action in real time eliminates this problem entirely.
The gap in hospital incident response coordination is not a skills gap and not a motivation gap. It is an infrastructure gap. The tools available to most hospitals were built to broadcast alerts, not to coordinate responses. Closing the gap requires a different category of tool.
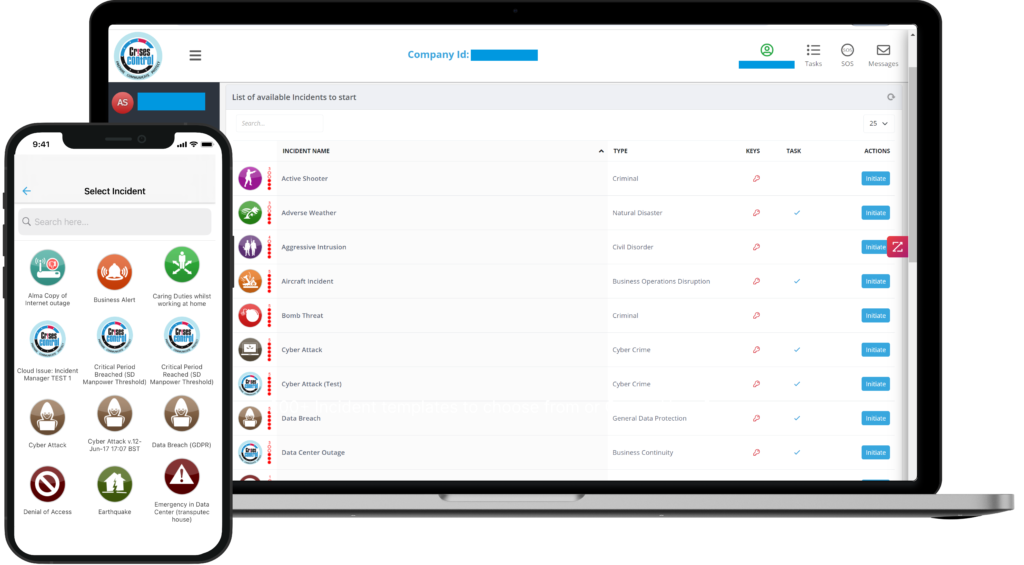
Interested in our Incident Management Software?
Flexible Incident Management Software to keep you connected and in control.
What Good Hospital Incident Response Coordination Looks Like
The right coordination infrastructure changes what happens in those 60 to 90 seconds after the alert fires.
- Role-based task assignment on the current shift
Instead of broadcasting to a group, the platform sends a specific task to whoever currently holds each relevant role on the active shift. The crash cart task goes to the crash cart team member who is on right now, not to whoever was named in the plan last quarter. The PING notification system delivers these role-specific alerts across SMS, voice, push, and email simultaneously. Acknowledgement is tracked individually. If the respiratory therapist does not respond within 60 seconds, the platform automatically escalates to her backup.
- A live coordination dashboard for every decision-maker
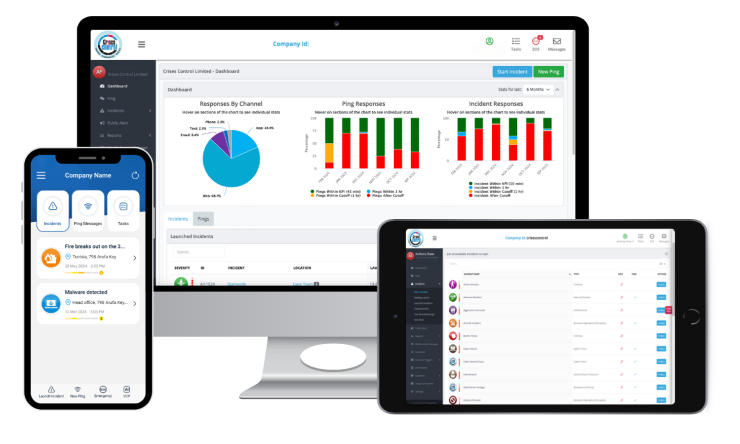
The incident coordinator, the charge nurse, the department head, and the hospital administrator all need the same real-time picture: who has acknowledged, who has not, what has been completed, what is still outstanding. The incident management platform provides a single live dashboard accessible on any device, updated in real time. Nobody needs to make a phone call to find out what is happening. The picture is always current.
- Automatic escalation without human intervention
When a task is not acknowledged within the configured window, the platform escalates automatically to the designated backup. This removes the human bottleneck from escalation entirely. The incident coordinator does not have to notice the gap, decide to act, and find the backup number. The system does it.
- Documentation that builds itself
Every notification sent, every acknowledgement received, every escalation triggered, every task completed: logged automatically with a timestamp as the incident unfolds. By the time the incident closes, the compliance record exists as a complete, accurate account of what happened. No reconstruction. No gaps. This is what good incident management software delivers as a baseline.
How Crises Control Delivers Hospital Incident Response Coordination
Crises Control is built for the specific conditions of hospital incident response coordination: shift-based staffing, multi-site networks, patient safety obligations, and regulatory documentation requirements that persist long after the incident is over.
When an incident is declared, PING delivers role-specific alerts across SMS, voice, push, and email simultaneously. Each person receives a specific task, not a generic alert. Acknowledgement is tracked individually. Non-responses escalate automatically to the backup role without any human intervention required.
The incident management platform gives every decision-maker the same live operational picture on a single dashboard. Every action is logged automatically as the incident unfolds. The CMS and Joint Commission compliance record is complete by the time the incident closes.
The platform operates on its own cloud infrastructure, independent of hospital IT systems. When internal networks are affected by the incident, the coordination platform keeps running.
To see this against your facility’s specific scenarios, request a demo.
FAQs
1. What is a hospital emergency communication system?
A hospital emergency communication system is the platform that manages how a hospital alerts, coordinates, and documents its response to a critical event. In a Code Blue scenario, it delivers role-specific notifications to the crash cart team, the on-call physician, and support staff, tracks who has acknowledged, escalates automatically when someone does not respond, gives the incident coordinator a live view of the response, and logs every action with a timestamp for compliance documentation. It is different from a basic overhead page or group text system because it coordinates the response rather than simply announcing the event.
2. Why does hospital incident response coordination fail even when notifications work?
Because notification tools were built to broadcast messages, not to coordinate responses. When an alert goes to a group, each member assumes someone else is handling it. There is no individual task ownership, no acknowledgement tracking, no automatic escalation, and no live shared picture for decision-makers. The alert reached everyone. Nothing coordinated what they did next. Fixing coordination requires a different layer of infrastructure on top of the notification system.
3. How does role-based task assignment improve hospital incident response?
Role-based task assignment routes response actions to whoever currently holds each relevant role on the active shift, rather than to named individuals who may be unavailable or off-site. When the primary role holder does not acknowledge within a configured window, the task escalates automatically to the backup for that role. This removes two failure points: the outdated contact list problem and the manual escalation bottleneck. The right person receives the task regardless of who is listed in the emergency plan.
4. What is the difference between hospital notification software and incident coordination software?
Notification software sends alerts and confirms delivery. Incident coordination software does everything that follows: it assigns tasks to active shift roles, tracks individual acknowledgements, escalates automatically when someone does not respond, activates predefined response workflows, provides a live dashboard for every decision-maker, and builds a complete compliance record as the incident unfolds. In hospital emergency response, both are needed. The notification starts the response. The coordination software runs it.
5. How does incident response coordination support Joint Commission and CMS compliance?
Joint Commission emergency management standards require hospitals to demonstrate that they can reach all relevant staff, confirm receipt, and produce audit documentation on demand during surveys. CMS Conditions of Participation require documented emergency communication plans with evidence that they function. A coordination platform that logs every notification, acknowledgement, escalation, and task completion automatically with timestamps provides this documentation as a byproduct of the incident response. When a surveyor asks to see your communication records from last month’s Code Blue, you produce them in under a minute. For more on the full healthcare mass notification framework this sits within, see the linked guide.